Direction
DRUG & ALCOHOL TREATMENT IN SAN DIEGO REHAB CENTER - ATON CENTER
Truly Individualized Care
Medically Assisted Detox. We ensure that you will have a safe and supportive environment for your detox. When you arrive at AToN Center, you will meet with the physician to review your individualized detox protocols. We have 24/7 nursing on-site to oversee this critical step in treatment with compassionate care.
Five Individual Therapy Sessions Per Week. Meet with an AToN Center Clinical team member one-on-one for counseling to target the underlying issues or co-occurring disorders such as anxiety, depression, and trauma resulting in substance misuse.
Alternatives to 12-Step and 12-Step Program. We believe there is no one size fits all approach to recovery. We believe in collaborating with residents to achieve a recovery philosophy that works in their life. This may include completing the 12-step program in your recovery or following an alternative method. Residents can choose the community support group that resonates more with them.
Luxury Lifestyle Amenities
Three individual Holistic Treatment sessions per week. We believe in treating the mind, body, and soul. Residents can choose from a holistic service menu such as massage, acupuncture, yoga, and personal training. Unlimited group holistic activities include sound bowl healing, breathwork, meditation, hiking, boot camp, yoga, and painting class.
On-site Chefs. Our chefs prepare healthy and delicious meals daily. During your intake, you will go over your specific dietary needs. The culinary team seeks to keep your preferences in mind.
Tropical surroundings and well-appointed rooms. Every home has a jacuzzi and pool, along with lush gardens. Every room is a space where you can have privacy, relaxation, comfort, and quiet. However, we encourage individuals to enjoy the outdoors and create community with their housemates.
INSURANCE ACCEPTED
AToN provides the highest level of care and can work with most insurance providers’ PPO plans. We are IN-NETWORK with Anthem. We believe deciding to go to treatment is one of the most important decisions an individual will make. Our staff understands financial limitations and will do our best to determine the best option to fit your circumstances.
WE ALSO ACCEPT MOST PPO PLANS WITH OUT-OF-NETWORK BENEFITS INCLUDING
CIGNA
UMR
MULTIPLAN
UNITED HEALTHCARE
OPTUM
AETNA
GEHA
EFFECTIVE TREATMENT
Detox at ATon. Our San Diego rehab for alcohol and drug addiction provides comfortable and safe detoxification as an essential component of treatment. With a 3 staff to 1 resident ratio, you’ll receive the individualized care and attention you deserve while recovering from withdrawal. We offer medical detox from alcohol, benzodiazepines, and opiates.
Stay for luxury residential treatment. After detox, it’ll be a smooth transition to inpatient treatment. At AToN, we use a combination of Western recovery practices and Eastern holistic healing techniques to provide the most comprehensive care for our residents. These treatment options help achieve overall wellness, including your physical, emotional, and mental health.
Treat your mind, body and spirit. Our team of counselors, holistic doctors, and medical professionals at this luxury rehabilitation center help residents recover and find new ways to live outside of our center. Holistic therapies focus on the root cause of substance misuse and heal a person wholly –mind, body, and spirit.
We also offer evidence-based therapies. This includes cognitive behavior therapy, dialectical behavior therapy, EMDR, trauma treatment, and mindfulness therapies. Therapeutic treatment is available individually and in groups to help residents understand addiction and find healthy ways to cope.
Learn relapse prevention methods. The team at AToN Center prioritizes a full recovery and provides each resident with relapse-prevention tools. After completing our treatment program in San Diego, you receive professional recommendations, consultations, and support services to ensure your recovery is just as successful outside of our luxury facility.
The AToN Difference
AToN is located on a private, 10-acre sanctuary.
Nestled within a secluded ten-acre sanctuary, AToN Center offers a serene escape surrounded by lush trees and tranquil waterfalls.
Our expansive grounds encompass five distinct estates, each providing an intimate setting for your recovery journey.
With a maximum of six residents per house, you can expect personalized attention and support tailored to your needs.
Our commitment to small group sizes ensures a close-knit community where individuals can feel comfortable and supported.
At AToN Center, our evidence-based curriculum is founded on principles of cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), and acceptance and commitment therapy (ACT).
In addition to these proven modalities, we incorporate techniques from mindfulness to promote holistic healing and personal growth.
Through our comprehensive approach, we empower residents to develop essential coping skills and cultivate lasting change in their lives.
We call all individuals at AToN Center: Residents
At AToN Center, we view you as more than a client—you are a valued member of our community.
That’s why we refer to you as a resident: Our facility becomes your home away from home during your time with us.
Here, you’ll find a warm and welcoming environment where you can feel safe, supported, and empowered to embark on your journey to recovery.
Our commitment to using inclusive language is just one of the ways we demonstrate our dedication to creating a supportive and stigma-free environment.
By referring to you as a resident, we emphasize the sense of belonging and camaraderie that permeates our facility. We want you to feel respected and valued for who you are without judgment or stigma.
Throughout your stay, you’ll receive unwavering support from our dedicated professionals. From our compassionate counselors to our experienced medical staff, everyone at AToN Center supports you every step of the way.
Whether you need assistance with treatment planning, emotional support, or practical guidance, we’re here to help you navigate your journey to recovery with confidence and dignity.
By using inclusive language and fostering a supportive environment, we ensure you feel safe, respected, and fully supported throughout your time at AToN Center.
We aim to empower you to achieve lasting sobriety and reclaim your life, one step at a time.
3 Clinician Treatment Team
At AToN Center’s San Diego rehabilitation facility, we are committed to providing personalized and effective treatment for individuals grappling with drug and alcohol addiction.
Central to our approach is maintaining a high Clinician to Resident ratio, ensuring that each resident receives the attention and support they need on a daily basis.
This individualized treatment model allows our clinicians to closely monitor progress, address concerns promptly, and tailor interventions to meet the specific needs of each client.
Recognizing that there is no one-size-fits-all approach to recovery, we offer a diverse range of evidence-based addiction treatment methods.
Our comprehensive treatment approach incorporates various modalities, including cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), motivational interviewing, Eye Movement Desensitization and Reprocessing (EMDR), Internal Family Systems (IFS) and mindfulness-based interventions.
These therapeutic techniques are selected based on each client’s individual needs and preferences to provide a customized and practical treatment experience.
In addition to addressing a client’s substance use disorder, we also recognize the importance of addressing their co-occurring mental health diagnosis.
Many individuals struggling with addiction may also experience underlying mental health concerns such as depression, anxiety, or trauma.
Our integrated approach to care ensures that these dual diagnoses are addressed concurrently, with specialized interventions and support services tailored to each client’s unique needs.
By providing comprehensive care that addresses both substance use and mental health concerns, we empower our clients to achieve lasting recovery and improved overall well-being.
Our holistic approach is very effective
At AToN Center, our holistic approach is rooted in the belief that true healing involves addressing the interconnected aspects of mind, body, and spirit. We understand that substance use disorders often co-occur with mental health conditions such as depression or anxiety, and our comprehensive approach is designed to address these complex challenges.
Through our holistic healing programs, we offer a diverse array of therapeutic modalities that cater to the varied needs of our residents. Outdoor activities, such as hiking or nature walks, provide opportunities for physical exercise and connection with the natural world, promoting mental clarity and emotional well-being. Our yoga and meditation sessions offer residents a chance to cultivate mindfulness, reduce stress, and develop inner peace and resilience.
In addition to these activities, acupuncture is available as a complementary therapy to promote relaxation, reduce cravings, and restore balance to the body’s energy systems. Other holistic modalities, such as massage therapy or art class, provide residents with creative outlets for self-expression and emotional processing.
By integrating these holistic approaches into our treatment program, we aim to support the overall well-being and recovery of our residents. Our holistic healing programs empower individuals to reconnect with themselves, cultivate inner resources for healing, and embark on a journey towards lasting wellness and sobriety.
We personally reach out to identified family members on behalf of our residents
At AToN Center, we understand the critical role that family support plays in the recovery process.
To facilitate this support, we take proactive steps to reach out to identified family members on behalf of our residents.
Through personalized outreach efforts, we aim to establish open lines of communication and foster the development of a robust support system within the identified family unit.
Our dedicated staff members engage in meaningful conversations with family members, offering guidance, education, and resources to help them better understand their loved one’s journey to recovery.
In addition to individualized outreach, we offer structured family sessions as part of our comprehensive treatment program.
These sessions provide a safe and supportive space for residents and their families to come together and address the challenges and dynamics associated with substance use disorders.
Led by experienced therapists and counselors, these sessions offer valuable insights into addiction, communication techniques, and strategies for supporting a loved one in recovery.
Through these collaborative efforts, families gain a deeper understanding of addiction and learn effective ways to provide support and encouragement to their loved one on their path to healing.
We provide personalized care even after you complete a program.
In our drug and alcohol rehab center, residents benefit from a comprehensive aftercare program designed to support their ongoing recovery journey.
Beyond their time in treatment, residents will receive phone calls from our dedicated staff, providing continued encouragement and guidance as they navigate life outside the center.
Additionally, residents are encouraged to participate in AToN aftercare, offering a supportive environment where they can connect with peers and share experiences.
To further nurture the sense of community and support, we organize special alumni events, providing opportunities for past and current residents to reunite and strengthen their bonds.
These gatherings serve as valuable resources for our AToN family to stay connected, share insights, and offer mutual support, contributing to the maintenance of long-term sobriety for all members.
We coordinate outpatient care for each resident
At AToN Center, our commitment to your recovery journey extends beyond the completion of our residential treatment program in southern California. We understand that transitioning back into everyday life can be challenging, which is why we offer continued support to ensure you remain on the path to lasting sobriety.
Our dedicated team works closely with you to help find the most suitable continuation of care options tailored to your specific needs and circumstances.
Whether it’s transitioning to sober living, enrolling in a Partial Hospitalization Program (PHP), or participating in Intensive Outpatient Program (IOP) services for outpatient treatment, we provide guidance and assistance every step of the way.
We believe that a smooth transition to ongoing care is essential for your successful recovery. By offering continued support and access to comprehensive treatment options, we empower you to maintain the progress you’ve made during your time with us and continue building a fulfilling life in sobriety.
Your recovery journey doesn’t end when you leave our doors – we’re here to support you every step of the way as you navigate the road to long-term wellness and happiness.
Yes, you can keep your phone!
While some addiction treatment centers impose strict restrictions on the use of phones, computers, and electronic devices, we take a different approach at AToN Center.
During your stay with us, there is no blackout period for using cell phones, tablets, or laptops.
We understand the importance of staying connected with loved ones, and we actively encourage individuals to maintain communication throughout their treatment journey.
At AToN Center, we recognize that the support of family and friends plays a crucial role in the recovery process. Rather than isolating residents from the outside world, we believe that maintaining open lines of communication can provide invaluable support and encouragement during this challenging time.
Whether it’s checking in with loved ones, seeking guidance from a sponsor, or accessing online resources for support, we empower our residents to utilize electronic devices as tools for connection and support.
Our approach reflects our commitment to fostering a supportive and inclusive environment where individuals feel empowered to make meaningful connections and engage in their recovery journey on their own terms.
By embracing technology and encouraging communication, we strive to create a treatment experience that is both effective and empowering, setting the stage for long-term success and wellness.
More About Our Treatment Program
-
FAQ
-
Play Video about AToN Video Overlay | AToN CenterWatch video for our frequently asked questions about admissions and AToN Center
-
Areas We Serve
-
AToN is Located in San Diego, California. We Accept Residents from all over the United States.
-
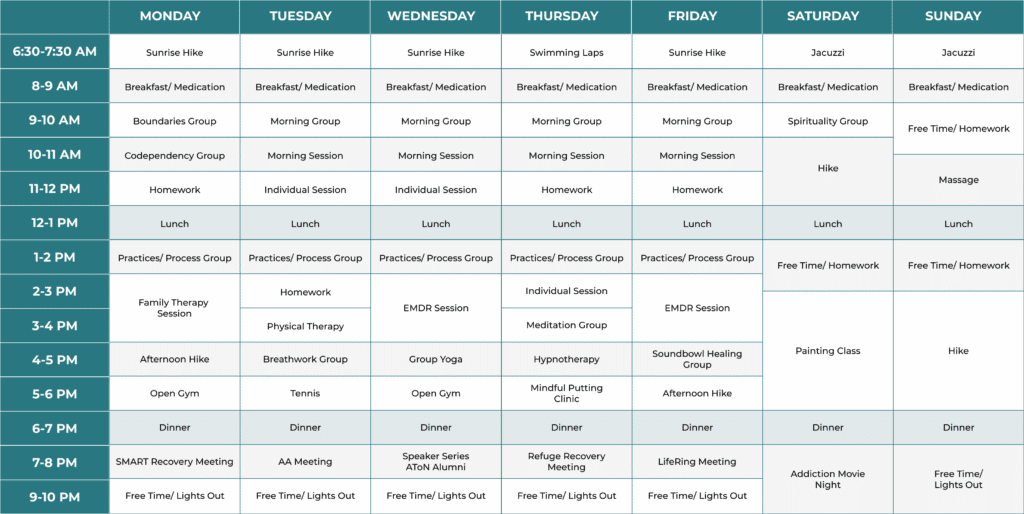
Daily Schedule
-
The individualized treatment plan our team of medical professionals creates for you follows a schedule with activities and counseling sessions to fill each day. Here is a sample schedule to give you an idea of what’s available at our treatment center in San Diego, California. The structure of a daily schedule benefits mental health and physical health, and is an essential component of drug and alcohol treatment.
-
What We Treat
-
Our comprehensive drug and alcohol treatment at our San Diego rehab center provides detox and therapeutic sessions for these substances:
-
Individualized Care
-
AToN Center’s San Diego rehab is a sanctuary staffed with highly trained psychologists and recovery personnel that offers an addiction recovery program.
AToN Center’s high Clinician to Resident ratio (1:2) allows for daily individualized treatment for those seeking respite from problematic drug and alcohol misuse.
AToN Center recognizes that a single modality doesn’t successfully meet the needs of every individual that is seeking recovery, therefore we offer a multitude of best practice addiction treatment methods in order to capture the needs of each client, including those with co-occurring mental health diagnoses.
The individualized treatment plan our team of medical professionals creates for you follows a schedule with activities and counseling sessions to fill each day. Here is a sample schedule to give you an idea of what’s available at our treatment center in San Diego, California. The structure of a daily schedule benefits mental health and physical health, and is an essential component of drug and alcohol treatment.
Our comprehensive drug and alcohol treatment at our San Diego rehab center provides detox and therapeutic sessions for these substances:
AToN Center’s San Diego rehab is a sanctuary staffed with highly trained psychologists and recovery personnel that offers an addiction recovery program.
AToN Center’s high Clinician to Resident ratio (1:2) allows for daily individualized treatment for those seeking respite from problematic drug and alcohol misuse.
AToN Center recognizes that a single modality doesn’t successfully meet the needs of every individual that is seeking recovery, therefore we offer a multitude of best practice addiction treatment methods in order to capture the needs of each client, including those with co-occurring mental health diagnoses.
Meet Our Staff
Dr. Rachel Conway
Dr. Rachel Conway
Dr. Leslie Sanders
Dr. Leslie Sanders
Dr. Kevin Murphy
Dr. Kevin Murphy
CHRIS MCDUFFIE
Dr. Kevin Murphy
Testimonials







The AToN Center has changed my life! From the amazing amenities, healthy food options, caring staff, and variety of treatment options, I can’t say more about how much I enjoyed my experience. They truly care about making a difference and helping someone get sober.
Choosing AToN Drug Rehab was the best decision I made. I learned about my depression and my addiction. I needed this – my family needed this. I hope I never have to send someone to a rehab but is I do – this is the only place I would send them.